CERVICAL CANCER: THE BASICS
In 2023, it’s estimated that 14,000 women will be diagnosed with cervical cancer and an estimated 4000 will die from it. Hispanic women have the highest likelihood of developing cervical cancer and black women are the most likely to die from it. But here’s the good news – increasing vaccination rates and routine screening can reduce the risk of cervical cancer by 90%!
Almost all cervical cancer cases (99%) are linked to infection with high risk human papillomavirus (HPV), an extremely common virus transmitted through sexual contact. Although most infections with HPV resolve spontaneously and cause no symptoms, persistent infection can cause cervical cancer in women.
SYMPTOMS
Early-stage cervical cancer has no signs or symptoms which is why regular screening with pap smears and HPV testing is critical. Advanced cervical cancer may present with abnormal vaginal bleeding, abnormal vaginal discharge or pelvic pain.
TYPES OF CERVICAL CANCER
Squamous cell carcinoma:
Most cervical cancers (up to 90%) are squamous cell carcinomas. These cancers develop from cells in the ectocervix or outer portion of the cervix.
Adenocarcinoma:
Cervical adenocarcinomas develop in the glandular cells of the endocervix or inner portion of the cervix.
RISK FACTORS
- Humanpapilloma virus infection
- Many sexual partners
- Early sexual activity
- Other sexually transmitted infections, especially HIV
- A weakened immune system (ie, following organ transplant)
- Smoking
- In utero exposure to diethylstilbestrol (DES)
PREVENTION
Since HPV is the most common cause of cervical cancer, the #1 step to prevent cervical cancer is to protect yourself from this viral infection!
GARDASIL 9 EXPANDED FOR PATIENTS AGED 27-45 YEARS OLD
- HPV vaccination, also known as Gardasil 9, is now available up to age 45! Check out our post from a few years ago (link above)
- Routine pap smears
- Minimize sexual partners and initiate intercourse later in life
- Avoid tobacco use
- Maintain a healthy immune system
If you’re overdue for your annual exam and/or think you are a candidate for the Gardasil vaccine, call us at 202-449-9570 to set up a visit with one of our Bloom Ob/Gyn providers!
CERVICAL CANCER: CAUSES Human Papillomavirus (HPV)
A person with HPV can pass the infection to someone without signs or symptoms
The Centers for Disease Control and Prevention or CDC estimates that there were 43 million HPV infections in 2018. 13 million of these represented new infections. This viral infection is so common,
in fact, that almost every sexually active person will get HPV at some point in their life. Since the virus is sexually transmitted, you can get HPV by having vaginal, anal, or oral sex with anyone who has the virus, even if you’ve only had one sexual partner. While it is most commonly spread during vaginal or anal sex, HPV also spreads through close skin-to-skin contact with any intimate contact.
In most cases (9 out of 10), HPV goes away on its own within two years without health problems
Fortunately, the majority of HPV infections are asymptomatic and resolve spontaneously without treatment or intervention. You can develop symptoms years after having sex with someone who has an infection, and this makes it hard to know when you were first exposed. Persistent infections can result in anogenital warts, precancers, and cervical, anogenital, or oropharyngeal cancers in women and men.
When HPV does not go away, it can cause cancer
There are over 100 different strains of the virus and different strains cause different types of disease:
HPV 6 and HPV 11 are two of the viral strains associated with genital warts – these viral strains (among others) are known as low risk strains as they are not associated with cancer
HPV 16 and HPV 18 are responsible for most cervical cancers – these viral strains (among others) are known as high risk strains as they are associated with cancer
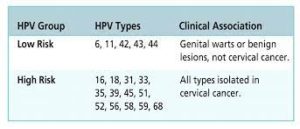
Infection with a high risk HPV strain is considered necessary for the development of cervical cancer, but by itself is not sufficient to cause cancer. The vast majority of women with HPV infection, even those with high-risk HPV types, do not develop cancer.
CERVICAL CANCER: SCREENING & DIAGNOSIS
George Papanicolaou was a pioneer in cytopathology and creator of the Papanicolaou test or “Pap smear”. He first published a study in 1928 outlining the different microscopic cellular structures of normal female reproductive cells compared to malignant or cancer cells. Ongoing research and study resulted in a landmark publication in 1943 that revolutionized the early detection of cervical cancer and, thus, the Pap test. It led to a 70% reduction in cervical cancer deaths and is still one of our current screening methods. The other principal screening tool for cervical cancer is a Human Papillomavirus or HPV test on the cells of the cervix.
How is a Pap test different from HPV screening?
A Pap test evaluates the actual cells on your cervix. During a pelvic exam, a brush is used to collect these cells which are then sent to a lab for review. A Pathologist examines the cells under a microscope and issues a report with their findings – either normal cells or abnormal cells with different levels of abnormality.
The HPV screen can be done at the same time as a Pap test (or on its own), but the technology is different. The lab looks for DNA from different HPV strains in those same cells as your Pap test. The presence of DNA indicates an infection with the virus. When these tests are run together, we call that “co-testing” and this is the common recommendation for cervical cancer screening.
When does cervical cancer screening start? And how often is it done?
Cervical cancer is very rare under age 21 and the current recommendation is to start screening for cervical cancer at that age. Co-testing typically starts at 30 years old. The frequency of testing varies. Your personal history, current medical concerns and the results of previous Pap tests and HPV screens determine the schedule. For instance, recommendations range from every 6 months to every 5 years depending on those factors.
What is colposcopy?
If your Pap test is abnormal or the HPV screen is positive, repeat testing may be recommended. Or you may be asked to schedule a colposcopy.
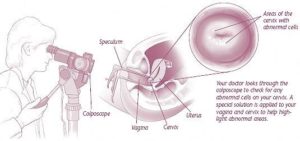
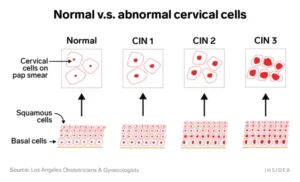
The biopsies are sent to the laboratory where a Pathologist can determine the level of abnormality present within the cells of the cervix. These abnormalities are “graded” as normal, grade 1, grade 2, grade 3 or invasive cancer. Grades 1 through 3 are known as cervical intraepithelial neoplasia or “CIN.”
CERVICAL CANCER: PREVENTION
Human Papillomavirus (HPV) vaccine
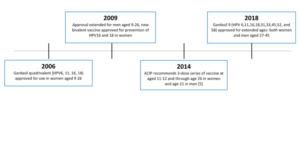
In 2009, the FDA approved another vaccine, Cervarix. This vaccine protects against two high-risk strains of HPV. Also in 2009, ACIP extended its HPV vaccine recommendation to include boys and men aged 9 – 26 years old.
Gardasil 9 protects against 9 strains of HPV Low-risk strains: 6, 11 High-risk stains: 16, 18, 31, 33, 45, 52, and 58
Gardasil 9, our current HPV vaccine, was approved in 2014. It protects against nine HPV strains, including high-risk types associated with cancer and low-risk types associated with genital warts. While still available worldwide, Gardasil 4 and Cervarix were discontinued in the United States in 2014.
In 2018, Gardasil 9 was approved for use in both women and men ages 27 – 45 years old
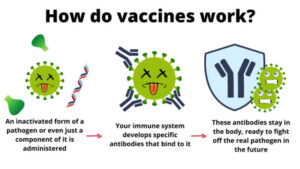
What is the HPV vaccine schedule?
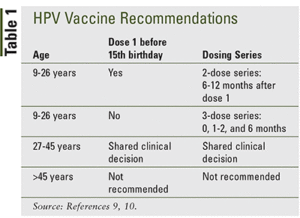
Catch-up vaccination (ie, receiving the remaining doses in a series if someone falls off track with their timeline and is not adequately vaccinated) is recommended for all persons through age 26 years old. Catch-up HPV vaccination is not recommended for adults older than age 26 years old since the health benefits of vaccination in this age range is minimal.
HPV vaccines are not licensed for use in persons older than age 45 years old and, for those age 27 – 45 years old who have not previously received the vaccine, it’s recommended to discuss with your provider the potential benefits based on your risk of exposure
What are the side effects of the HPV vaccine?
While many people who get the HPV vaccine have no side effects at all, some report having very mild side effects. The most common side effects of the HPV vaccine are include:
- Pain, redness, or swelling in the arm where the shot was given
- Fever
- Dizziness or fainting (fainting after any vaccine, including HPV vaccine, is more common among adolescents than others)
- Headache or feeling tired
- Nausea
- Muscle or joint pain
To prevent fainting and injuries from fainting, adolescents should be seated or lying down during vaccination and for 15 minutes after getting the shot.
Very rarely, severe (anaphylactic) allergic reactions might occur after vaccination.