Breast health is something every woman thinks about at some point; whether it’s navigating puberty, breastfeeding, dealing with hormonal changes, or thinking about mammograms. Your breasts change throughout your life, and knowing what’s normal (and what’s not) can help you feel more confident about your body and more prepared to protect your health.
Understanding Breast Changes Through the Years
Your breasts are constantly responding to your body’s hormonal shifts. It’s normal for them to feel different at various life stages. Understanding what’s typical at each age can help you identify when something may need attention by your provider.
Adolescence and Early Adulthood (Teens to 20s)
Puberty brings major changes, including the development of breast tissue. During this time, it’s common to experience breast tenderness/soreness, lumpiness, and changes related to the menstrual cycle. These are usually due to shifting hormone levels and are rarely cause for concern.
By your late teens and early twenties, your breast tissue will have matured. While the risk of breast cancer is low at this age, it’s still important to become familiar with how your breasts normally look and feel. That way, you can more easily notice if something changes or feels different.
We typically do not recommend routine mammograms in this age group unless there is a strong family history of breast cancer or a genetic risk.
Reproductive Years (20s to 40s)
During your 20s and 30s, breast tissue continues to change in response to hormone fluctuations, birth control use, pregnancy, and breastfeeding. You may notice swelling or tenderness before your period or during early pregnancy.
If you’re breastfeeding, it’s common to develop clogged ducts or experience mastitis, an infection that causes redness, warmth, and pain. Let your provider know if symptoms persist, as they may need treatment.
Breast self-awareness is key during these years. It’s a good time to start paying closer attention to your breast health by noting any new lumps, skin changes (such as dimpling), or discharge from the nipples.
Routine clinical breast exams may be part of your annual well-woman visit. If you have a family history of breast cancer, your provider may recommend earlier or more frequent screenings.
Midlife and Menopause (40s to 60s)
This is the time when routine screening for breast cancer typically begins. Most guidelines recommend starting mammograms at age 40 and continuing yearly or every other year depending on your health history and provider recommendations.
During perimenopause and menopause, declining estrogen levels can lead to changes in breast density and sensitivity. Your breasts may feel less full or slightly softer than in earlier years.
If you’re taking hormone therapy to manage menopause symptoms, talk to your OB/GYN about how that may affect your breast health and screening schedule based on your age and risk factors.
Later Life (60s and Beyond)
Breast cancer risk increases with age, so continued screening is important into your 60s and 70s. The decision to continue mammograms beyond age 75 is individualized based on your overall health, life expectancy, and personal preference. Be sure to have this conversation with your provider to make informed decisions.
At this stage, some women may stop experiencing the same breast tenderness or hormonal symptoms from earlier decades. Even so, it’s still important to stay alert to any new lumps, skin changes, or nipple discharge.
What Is a Mammogram?
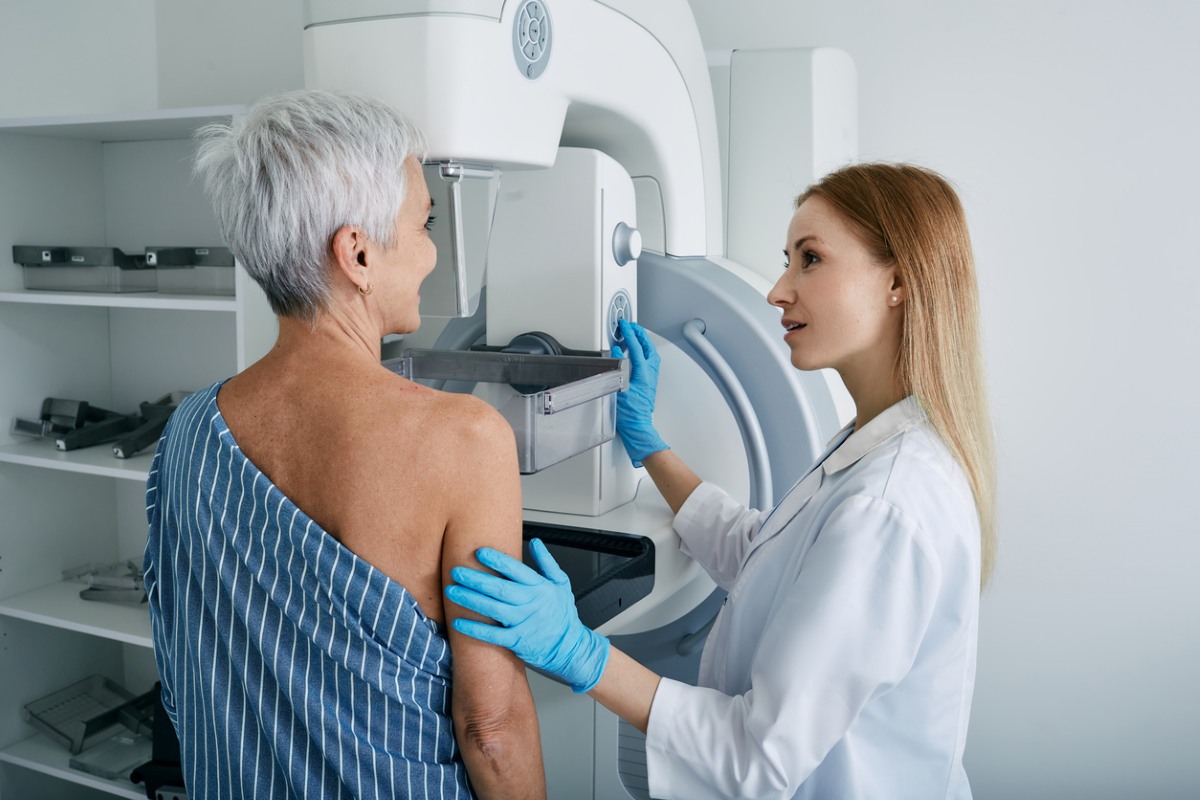
A mammogram is a specialized X-ray used to detect changes in breast tissue that may not be felt during a physical exam. It is the gold standard for early breast cancer detection and can find tumors that are too small to be felt by hand.
There are two types:
- Screening mammogram: Done routinely in women without symptoms to detect early signs of cancer.
- Diagnostic mammogram: Ordered when there are symptoms such as a lump or nipple discharge, or to follow up on abnormal results from a screening.
The procedure itself takes about 20 minutes. During the test, your breast will be gently compressed between two plates to spread the tissue evenly for imaging. While some women find the pressure uncomfortable, it is brief and not typically painful.
When Should You Start Breast Cancer Screening?
There is some variation in national guidelines, but many OB/GYNs, including those at Bloom, follow the recommendations of the American College of Obstetricians and Gynecologists (ACOG):
- Begin screening mammograms at age 40
- Repeat every 1 to 2 years depending on risk factors
- Continue as long as you are in good health and expect to live 10 or more years
If you have a strong family history of breast or ovarian cancer, or if you carry a BRCA gene mutation, your provider may suggest starting earlier or adding other imaging like breast MRI.
No matter when you start or stop, the most important thing is to stay consistent and talk to your provider about what’s right for your specific health profile. This is the best way to be an advocate for yourself and make an informed decision regarding your health.
Common Myths About Breast Health
There’s a lot of misinformation about breast cancer and mammograms. Let’s clear up a few common myths:
Myth: If you don’t have a family history of breast cancer, you’re not at risk.
Fact: Most women who develop breast cancer do not have a family history. Regular screenings are important for everyone.
Myth: Mammograms are only necessary if you feel a lump.
Fact: Mammograms detect changes long before a lump can be felt. Waiting for symptoms could delay diagnosis.
Myth: Mammograms are always painful.
Fact: Some discomfort is normal, but the test is quick. Communicate with your technician to make the process as comfortable as possible.
Myth: Only older women get breast cancer.
Fact: While risk increases with age, younger women can and do develop breast cancer. Awareness at every age is essential.
How Bloom OB/GYN Supports Breast Health
Your care at Bloom OB/GYN includes more than just reproductive health; we take a whole-person approach, and breast care is an important part of that. Here’s how we help support your breast health:
- Annual clinical breast exams during wellness visits
- Mammogram referrals with guidance on when and where to screen
- Evaluation of breast symptoms, such as lumps or pain
- Education on breast self-awareness and normal changes
- Risk assessment if you have a family history or other concerns
Know Your Breasts. Know Your Risk.
Being aware of your breast health starts with knowing what’s normal for your body. Regular self-checks, clinical exams, and mammograms work together to give you the full picture and be proactive with your help.
You don’t need to do formal self-breast exams on a strict schedule, but it’s helpful to check in with yourself regularly. Look for changes in size, shape, texture, or skin appearance. Pay attention to pain, swelling, nipple inversion, or discharge.
If something feels different or concerning, don’t wait. Reach out to your provider right away. Most changes are not cancer, but only a proper evaluation can determine the cause.
Take Charge of Your Breast Health Today
Your health evolves with each season of life, and so should your care. Whether you’re due for your first mammogram or simply want to understand what’s normal, Bloom OB/GYN is here to guide you with compassion, clarity, and clinical expertise. Schedule your next annual exam or breast screening referral today.