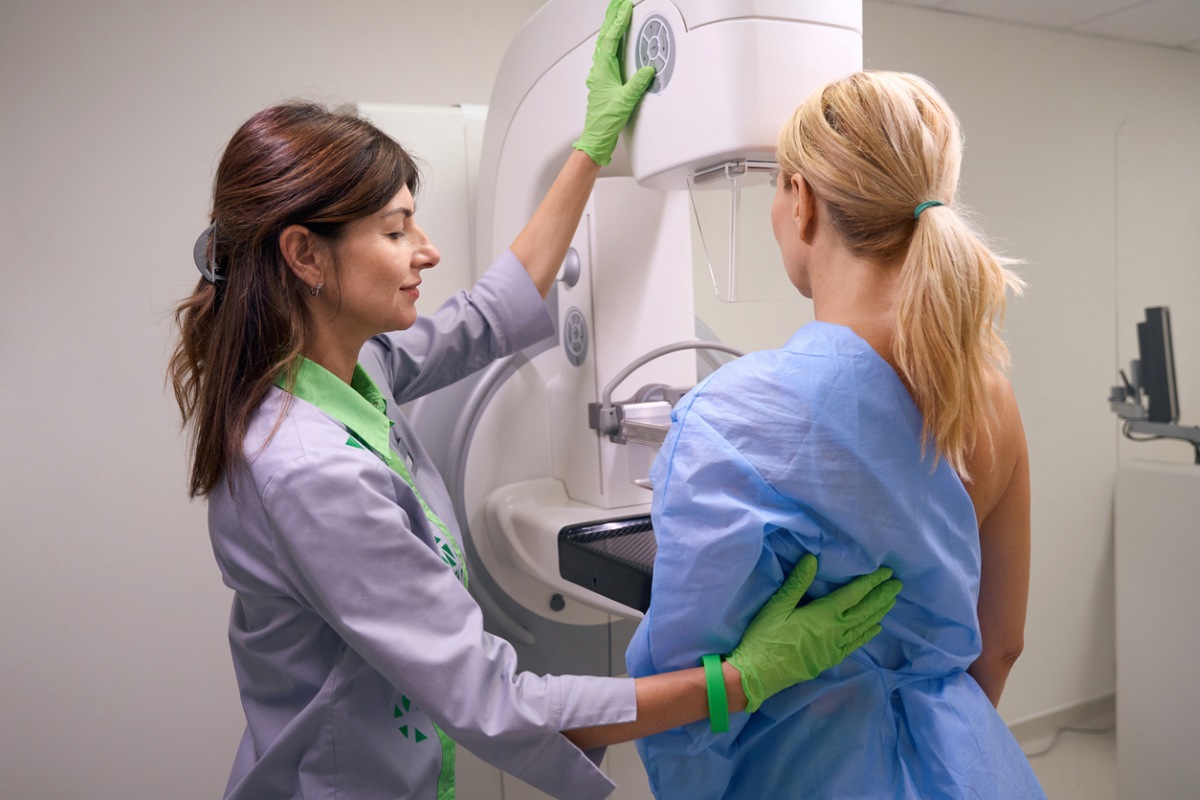
A mammogram is a low-dose X-ray of the breast used to detect cancer early, often before you can feel a lump or notice any changes. Screening mammograms are one of the most effective tools we have for catching breast cancer in its earliest and most treatable stages. With updated national guidelines now in place, the recommendations for when to start screening have shifted significantly.
What Changed and Why It Matters
In April 2024, the U.S. Preventive Services Task Force (USPSTF) updated its breast cancer screening guidelines to recommend that all women begin getting mammograms at age 40, with screenings every two years through age 74. Previously, the USPSTF recommended routine screening starting at age 50, with the option to begin earlier based on individual risk factors and personal preference.
The American College of Obstetricians and Gynecologists (ACOG) followed with its own update in October 2024, also recommending that all average-risk individuals start screening mammography at age 40. ACOG recommends screening every 1 to 2 years, with the exact frequency determined through a shared conversation between you and your provider.
Several factors drove these changes. Between 2015 and 2019, the rate of invasive breast cancer among women in their 40s increased by about 2% each year. Research also showed that starting screening earlier provides a greater overall benefit in reducing breast cancer deaths. The USPSTF estimates that beginning at age 40 rather than 50 could save nearly 20% more lives.
Who Should Get Screened?
These updated recommendations apply to women at average risk for breast cancer. You are considered average risk if you do not have a known genetic mutation like BRCA1 or BRCA2, a strong family history of breast or ovarian cancer, or a history of chest radiation at a young age. If you are unsure whether you should consider genetic testing, your provider can help you evaluate your risk.
If you do have any of these risk factors, your provider may recommend starting screening before age 40 or using additional imaging, such as breast MRI. That is why having an open conversation with your OB/GYN about your personal and family health history is so valuable. Your provider can help you understand your individual risk level and build a screening plan that makes sense for you.
What to Expect at Your Mammogram
If you have never had a mammogram before, knowing what to expect can help ease any nerves. On the day of your appointment, avoid wearing deodorant, lotion, or powder, as these products can interfere with the X-ray images.
During the exam, you will undress from the waist up and stand in front of the mammography machine. A technician will position one breast at a time between two flat plates, which briefly compress the tissue to obtain a clear image. The compression can feel uncomfortable or tight, but it only lasts a few seconds per image. The entire appointment typically takes about 20 minutes.
After your mammogram, a radiologist reviews the images and assigns a score. Most results come back normal and simply require you to continue routine screening. If something needs a closer look, your provider may recommend additional imaging or follow-up. A callback does not automatically mean cancer. It often just means the radiologist wants a clearer picture.
Why Early Detection Changes Outcomes
Breast cancer is the second most common cancer among women in the United States and the leading cause of cancer death among Black and Hispanic women. When breast cancer is found early through screening, it is highly treatable and often requires less aggressive treatment. Regular mammograms give you and your care team the best chance of catching any changes before they become more serious. Staying up to date with your gynecology visits is an important part of monitoring your overall health, including breast health.
Both the USPSTF and ACOG have also emphasized that earlier screening may help reduce racial disparities in breast cancer outcomes. Black women have the highest breast cancer mortality rate among all women, even when adjusting for age and stage at diagnosis. Starting screening at 40 across the board is one step toward closing that gap.
Your Breast Health Is Worth Prioritizing
Staying on top of your mammogram schedule is one of the simplest and most impactful things you can do for your long-term health. If you are 40 or older and have not yet scheduled your first mammogram, or if it has been more than two years since your last screening, now is a great time to take that step. Talk with your provider at Bloom OB/GYN about your breast health, your personal risk factors, and the screening schedule that is right for you. You can request an appointment by calling (202) 449-9570 or visiting bloom-obgyn.com/request-appointment.